Table of contents
What is Atherosclerosis?
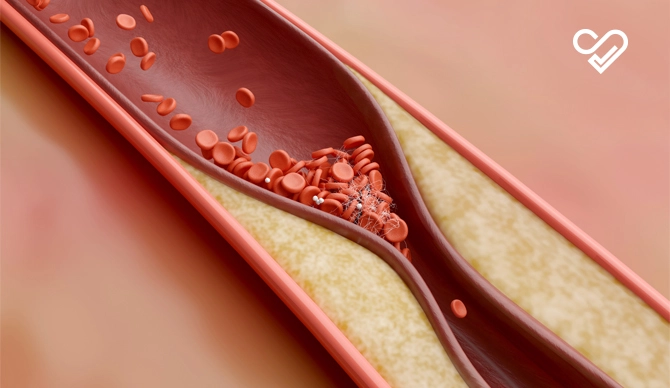
Atherosclerotic cardiovascular disease is a complex and progressive condition characterized by the buildup of plaque in the arteries, which then leads to the narrowing and hardening of these blood vessels.
This plaque that is made up of cholesterol, fat, calcium, and other substances, gradually gets collected along the walls of the arteries, disrupting the blood flow and increasing the risk of serious complications like heart attack and stroke.
Atherosclerosis Symptoms
While atherosclerotic cardiovascular disease typically develops silently over several years, it can eventually manifest in various atherosclerosis symptoms, including:
- Chest Pain (Angina): Angina, one of the hallmark atherosclerosis symptoms, occurs when narrowed or blocked arteries limit oxygen-rich blood flow to the heart muscle. It’s often described as pressure, tightness, or burning in the chest.
- Shortness of Breath: Atherosclerotic cardiovascular disease can reduce blood flow to the lungs, leading to shortness of breath, especially during physical exertion or even while lying flat. This atherosclerosis symptom, called dyspnea, results from the heart’s inability to pump enough blood to meet the body’s oxygen demands.
- Fatigue: Reduced blood flow to the heart muscle caused by atherosclerotic cardiovascular disease can lead to chronic fatigue or unexplained tiredness. The heart needs to work harder to pump oxygen-rich blood, resulting in feelings of weakness or exhaustion.
- Dizziness or Lightheadedness: Narrowing of arteries can disrupt blood flow to the brain, causing dizziness, lightheadedness, or fainting. These atherosclerosis symptoms, worsened by sudden movements, may indicate inadequate blood supply to the brain.
- Leg Pain While Walking (Claudication): Atherosclerotic cardiovascular disease in leg arteries can cause intermittent claudication i.e. cramping, weakness, or numbness during walking or physical activity.
- Numbness or Weakness in Extremities: Peripheral artery narrowing due to atherosclerotic cardiovascular disease can diminish blood flow to extremities, causing numbness, tingling, weakness, or coldness.
- Cognitive Impairment: Severe atherosclerotic cardiovascular disease in brain arteries can impair cognitive function, increasing stroke or transient ischemic attack (TIA) risk. Atherosclerosis symptoms include confusion, memory loss, difficulty speaking or understanding, and changes in vision or coordination.
Atherosclerosis Causes
Several factors contribute to the development of atherosclerotic cardiovascular disease – the list of these atherosclerosis causes include:
- High Cholesterol Levels: Elevated LDL cholesterol, known as “bad” cholesterol, is pivotal in the development of this condition. It infiltrates arterial walls, triggering inflammation and plaque formation.
- High Blood Pressure (Hypertension): Chronic hypertension stiffens and narrows arteries, accelerating plaque accumulation. This heightened pressure damages arterial walls.
- Smoking: Tobacco smoke’s harmful chemicals damage blood vessel linings, fuel inflammation, and expedite plaque formation. Smoking also lowers “good” HDL cholesterol levels.
- Diabetes: Poorly controlled diabetes raises blood sugar levels, promoting atherosclerotic cardiovascular disease via endothelial dysfunction, inflammation, and impaired lipid metabolism.
- Obesity: Excess visceral fat links to insulin resistance, inflammation, and dyslipidemia. Obesity also spurs pro-inflammatory cytokine release, further harming arteries.
- Sedentary Lifestyle: Physical inactivity hampers cardiovascular health, increasing the risk of atherosclerotic cardiovascular disease. Regular exercise bolsters blood pressure, cholesterol, and weight, while enhancing endothelial function and reducing inflammation.
- Unhealthy Diet: Diets rich in saturated fats, trans fats, and refined carbs drive atherosclerotic cardiovascular disease by fueling dyslipidemia, inflammation, and oxidative stress. On the other hand, diets that are abundant in fruits, veggies, whole grains, lean proteins, and healthy fats protect against this condition.
Atherosclerosis Diagnosis
Atherosclerosis diagnosis typically involves a combination of medical history review, physical examination, and diagnostic tests such as:
- Lipid profile
- Electrocardiogram (ECG)
- Stress test
- Echocardiogram
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Angiography
These tests help evaluate the extent of arterial blockages and assess the overall cardiovascular health of an individual.
Atherosclerosis Treatment
Atherosclerosis treatment aims to reduce plaque buildup, alleviate atherosclerosis symptoms, prevent complications, and improve overall cardiovascular health.
Atherosclerosis treatment options may include:
Lifestyle Modifications:
Adopting heart-healthy habits is key to atherosclerosis treatment. This includes a balanced diet rich in fruits, veggies, whole grains, and lean proteins, while limiting saturated fats, trans fats, cholesterol, and sodium. Regular exercise, smoking cessation, weight management, and stress reduction techniques also improve cardiovascular health and slow atherosclerotic cardiovascular disease.
Medications:
Several medications can be used for atherosclerosis treatment:
- Statins lower cholesterol, reducing plaque buildup.
- Antiplatelet agents like aspirin prevent blood clots in narrowed arteries.
- Blood pressure medications control hypertension, easing strain on the heart.
- Blood sugar control medications manage diabetes, reducing the complications.
Revascularization Procedures:
When atherosclerosis causes significant blockages, invasive procedures are used to restore blood flow:
- Angioplasty and stent placement open blocked arteries and keep them clear.
- Coronary artery bypass grafting (CABG) reroutes blood flow around blockages using grafts from other blood vessels.
Lifestyle Support Programs:
Cardiac rehabilitation programs guide individuals with atherosclerotic cardiovascular disease in maintaining heart-healthy lifestyles. These include supervised exercise, nutrition counseling, smoking cessation, stress management, and cardiovascular education.
Monitoring and Follow-Up:
Regular check-ups with healthcare providers are crucial for monitoring atherosclerosis. These appointments track disease progression, assess atherosclerosis treatment effectiveness, and adjust management plans as needed. Tests and lifestyle evaluations ensure optimal cardiovascular health and prevent complications.
– Disclaimer –
This blog is for informational & educational purposes only, and does not intend to substitute any professional medical advice or consultation. For any health related concerns, please consult with your physician, or call 911.