Do you ever feel your heart racing unexpectedly? Or perhaps moments where your heartbeat feels irregular?
These symptoms might be related to a condition known as Atrial Fibrillation (AFib) – a common heart rhythm disorder that affects millions worldwide.
But what is AFib, and how does it impact your health? – Let’s find out!
Table of contents
What is Atrial Fibrillation?
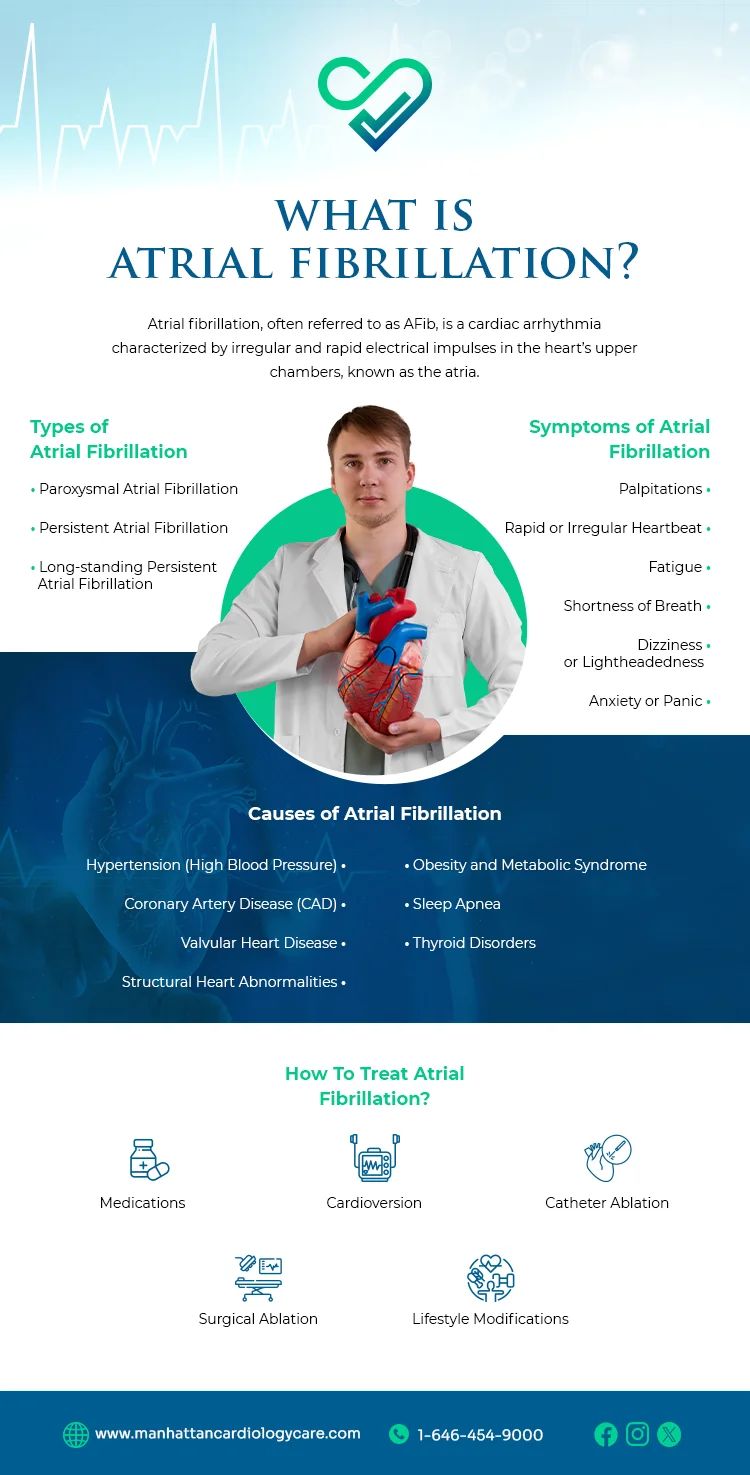
Atrial fibrillation, often referred to as AFib, is a cardiac arrhythmia characterized by irregular and rapid electrical impulses in the heart’s upper chambers, known as the atria. Instead of beating in a coordinated and rhythmic pattern, the atria fibrillates or quivers erratically, compromising the heart’s ability to pump blood efficiently.
Types of Atrial Fibrillation
Atrial fibrillation (AFib) occurs in various forms, and each type presents unique characteristics and implications for patient management.
Primary types of atrial fibrillation include:
- Paroxysmal Atrial Fibrillation: Paroxysmal AFib features intermittent episodes of irregular heart rhythm that spontaneously reverts to normal sinus rhythm within 7 days. While these episodes may occur infrequently or with varying frequency and duration, they impact quality of life and increase the risk of stroke and other complications.
- Persistent Atrial Fibrillation: Persistent AFib involves sustained irregular heart rhythm that lasts beyond 7 days, requiring medical intervention to restore normal sinus rhythm. Unlike paroxysmal AFib, persistent AFib does not self-terminate and often requires medications or even procedures like cardioversion to control and maintain heart rhythm.
- Long-standing Persistent Atrial Fibrillation: Long-standing persistent AFib is a subtype lasting over a year, posing greater challenges for rhythm control. Aggressive treatments like catheter ablation or surgery may be needed to restore sinus rhythm. Those with long-standing AFib face increased risks of stroke, heart failure, and other complications.
Symptoms of Atrial Fibrillation
Listed below are the common symptoms associated with atrial fibrillation:
- Palpitations: Palpitations are sensations of irregular or rapid heartbeat, described as pounding sensations in the chest. Patients with AFib may experience palpitations persistently.
- Rapid or Irregular Heartbeat: Individuals with AFib may perceive their heartbeats as unusually fast or irregular, causing discomfort or unease.
- Fatigue: Fatigue and weakness are common symptoms of AFib, attributed to the heart’s inefficiency in pumping blood.
- Shortness of Breath: AFib can disrupt the heart’s ability to maintain sufficient blood flow, leading to breathlessness, especially during physical activity, which may result from reduced cardiac output.
- Dizziness or Lightheadedness: Episodes of dizziness or lightheadedness may occur during AFib episodes. Reduced blood flow to the brain can cause temporary loss of balance or fainting spells.
- Anxiety or Panic: The irregular heartbeat in AFib can trigger feelings of anxiety or panic. Heightened awareness of palpitations or concerns about complications may lead to emotional distress.
Causes of Atrial Fibrillation
Atrial fibrillation (AFib) can occur due to various underlying factors. Here are the main causes associated with atrial fibrillation:
- Hypertension (High Blood Pressure): Hypertension significantly increases the risk of atrial fibrillation by causing structural changes in the heart and disrupting electrical conduction. Chronic hypertension leads to left ventricular hypertrophy, atrial dilation, and fibrosis, increasing susceptibility to AFib.
- Coronary Artery Disease (CAD): CAD, characterized by narrowed or blocked coronary arteries, heightens AFib risk by inducing myocardial remodeling and scar formation. Ischemic heart disease and myocardial infarction predispose individuals to arrhythmias like AFib.
- Valvular Heart Disease: Valvular heart disease, including mitral valve prolapse, mitral stenosis, or aortic valve disease, disrupts cardiac function and promotes AFib development. Valve abnormalities cause hemodynamic changes, atrial enlargement, and turbulent blood flow, fostering arrhythmia formation.
- Structural Heart Abnormalities: Structural heart defects like congenital defects, cardiomyopathies, or past cardiac surgeries increase AFib risk. Conditions such as atrial septal defects and hypertrophic cardiomyopathy alter heart structure, increasing the risk of arrhythmia.
- Obesity and Metabolic Syndrome: Obesity and metabolic syndrome heightens AFib risk through abdominal fat accumulation and associated metabolic disturbances. Pro-inflammatory factors secreted by adipose tissue contribute to atrial fibrosis, oxidative stress, and electrical remodeling, predisposing to AFib.
- Sleep Apnea: Obstructive sleep apnea raises AFib risk through intermittent hypoxia and autonomic dysfunction during sleep. Sympathetic activation and negative intrathoracic pressure promote atrial arrhythmogenesis, exacerbating AFib susceptibility.
- Thyroid Disorders: Thyroid disorders like hyperthyroidism or hypothyroidism disrupt normal cardiac function and raise AFib risk. Thyroid hormone imbalance alters heart contractility, heart rate, and rhythm.
- Other Contributing Factors: Additional AFib risk factors include aging, family history of arrhythmias, smoking, chronic kidney disease, diabetes mellitus, and certain medications like stimulants or antiarrhythmics.
How To Treat Atrial Fibrillation?
Atrial fibrillation (AFib) treatment aims to control symptoms, restore normal heart rhythm, prevent complications, and improve the overall quality of life. Treatment strategies for AFib may vary based on the type of arrhythmia, underlying causes, and individual patient factors.
Here are the treatment options available for atrial fibrillation:
- Medications: Medications are crucial for managing atrial fibrillation by controlling heart rate, restoring sinus rhythm, and preventing thromboembolic complications. Antiarrhythmic drugs like flecainide or amiodarone maintain sinus rhythm, while beta-blockers and calcium channel blockers slow heart rate during AFib episodes. Anticoagulants such as warfarin or novel oral anticoagulants (NOACs) like dabigatran prevent stroke.
- Cardioversion: Cardioversion restores normal sinus rhythm by delivering an electrical shock to the heart. It can be done electrically or pharmacologically using antiarrhythmic medications.
- Catheter Ablation: Catheter ablation eliminates abnormal electrical pathways in the heart to treat AFib. This minimally invasive procedure creates scar tissue in the heart, interrupting aberrant conduction pathways.
- Surgical Ablation: Surgical ablation, performed during open-heart surgery, creates scar tissue in the atria to disrupt abnormal electrical signals causing AFib. It’s reserved for patients undergoing cardiac surgery who haven’t responded to other treatments.
- Lifestyle Modifications: Heart-healthy habits, including a balanced diet, regular exercise, weight management, limited alcohol consumption, smoking cessation, and stress management, are vital for managing AFib and reducing symptoms.
– Disclaimer –
This blog is for informational & educational purposes only, and does not intend to substitute any professional medical advice or consultation. For any health related concerns, please consult with your physician, or call 911.