Table of contents
What is Peripheral Artery Disease?
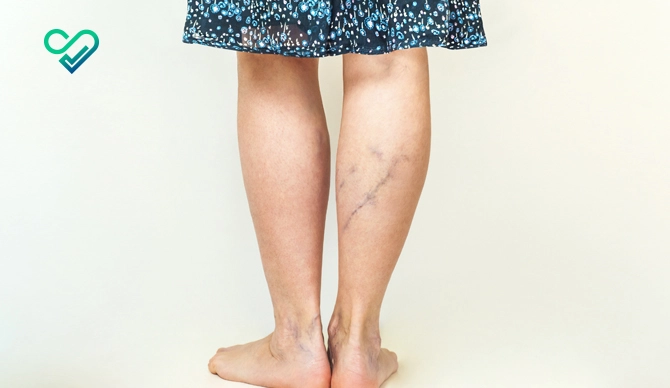
Peripheral Artery Disease (PAD) is a commonly occuring circulatory problem in which the blood flow to your limbs, mostly legs, is reduced due to the narrowed arteries, caused by the buildup of fatty deposits (plaques) within the artery walls. As a result, the affected limbs do not receive sufficient oxygen-rich blood, leading to various symptoms and complications.
How Common is Peripheral Artery Disease?
Peripheral Artery Disease affects millions of individuals worldwide, with the prevalence increasing with age. It is estimated that around 8.5 million people in the United States alone have PAD, although many cases remain undiagnosed.
What Are The Stages of Peripheral Artery Disease?
Peripheral Artery Disease typically progresses through four stages:
- Asymptomatic PAD:
In this stage, individuals do not experience any noticeable PAD symptoms. However, underlying arterial narrowing or blockages may already be present, increasing the risk of complications.
- Claudication (Intermittent Claudication):
Claudication refers to pain or cramping in the legs that occurs during a physical activity. This symptom arises due to reduced blood flow to the leg muscles, causing inadequate oxygen supply.
- Rest Pain:
Rest pain is characterized by persistent discomfort or pain in the legs, even while at rest. It often occurs during nighttime hours and can even disrupt sleep. Rest pain indicates more severe arterial blockages and compromised blood flow to the legs, leading to tissue ischemia.
- Critical Limb Ischemia:
Critical limb ischemia is the most advanced stage of Peripheral Artery Disease and is characterized by severe arterial blockages. PAD symptoms may include severe pain, non-healing wounds or ulcers, tissue necrosis (gangrene), and an increased risk of limb loss if left untreated.
Peripheral Artery Disease Symptoms
Peripheral Artery Disease symptoms can vary depending on the severity of the condition, but may include:
- Leg pain or cramping while walking (intermittent claudication)
- Numbness or weakness in the legs
- Coldness in the lower leg or foot
- Sores or wounds on the legs or feet that heal slowly or not at all
- Shiny skin on the legs
- Weak or absent pulses in the legs or feet
Peripheral Artery Disease Causes
The primary cause of Peripheral Artery Disease is atherosclerosis, a condition characterized by the buildup of plaque within the arteries. However, several factors can be listed among the Peripheral Artery Disease causes, including:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Obesity
- Family history of PAD or cardiovascular disease
Risk Factors For Peripheral Artery Disease
Several risk factors increase the likelihood of developing PAD, including:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Obesity
- Age (especially over 50)
- Family history of PAD or cardiovascular disease
Peripheral Artery Disease Diagnosis
Peripheral Artery Disease diagnosis typically involves a combination of medical history, physical examination, and specialized tests that not only diagnose but also help determine the extent of arterial blockage and guide treatment decisions.
- Medical History and Physical Examination: Initial diagnosis includes assessing medical history and risk factors like smoking, diabetes, hypertension, and hyperlipidemia. Peripheral Artery Disease symptoms such as weak pulses, cool skin, or slow-healing wounds may indicate PAD.
- Ankle-Brachial Index (ABI): ABI is a non-invasive test comparing ankle and arm blood pressure. Lower ABI values suggest reduced leg blood flow, indicating possible PAD.
- Doppler Ultrasound: This uses sound waves to assess artery blood flow, useful for detecting abnormalities like narrowing or blockages, especially in the legs.
- Angiography: This invasive procedure uses contrast dye and X-rays to visualize blood vessels, providing detailed information about artery blockages to guide Peripheral Artery Disease treatment decisions.
- CTA or MRA: These advanced imaging techniques create 3D images of blood vessels using CT or MRI, accurately identifying PAD-related abnormalities or blockages.
- Exercise Testing: Treadmill or bicycle tests evaluate claudication symptoms and functional impairment due to PAD, aiding in severity assessment and treatment planning.
- Blood Tests: These assess parameters like lipid levels, blood glucose, and inflammatory markers to identify PAD risk factors.
Peripheral Artery Disease Treatments
Peripheral Artery Disease treatments aim to relieve symptoms, improve blood flow, and reduce the risk of complications. Depending on the severity of the condition, treatment options may include:
- Lifestyle Modifications: Changes in habits like quitting smoking, adopting a healthy diet, maintaining a healthy weight, and regular exercise can help alleviate PAD symptoms and reduce progression.
- Medications: Prescribed drugs like antiplatelet agents (aspirin, clopidogrel), statins, and medications for blood pressure and blood sugar management can reduce PAD symptoms and lower risks.
- Peripheral Artery Angioplasty and Stenting: Minimally invasive procedures using a balloon catheter to widen narrowed arteries and sometimes placing a stent to maintain blood flow.
- Peripheral Artery Bypass Surgery: Surgical procedure using a healthy blood vessel to bypass blocked arteries, restoring proper blood flow to the affected limb.
- Atherectomy: Procedure to remove plaque buildup from arteries using specialized devices, improving blood flow.
- Exercise Therapy: Supervised exercise programs tailored to improve walking ability, reduce symptoms, and enhance cardiovascular health.
- Wound Care and Limb Salvage Techniques: Management of chronic wounds or ulcers with techniques like wound debridement, dressings, and offloading devices, or in severe cases, vascular reconstruction or amputation.
- Comprehensive Cardiovascular Care: Multidisciplinary approach involving various healthcare professionals to address risk factors, optimize therapy, and provide personalized treatment plans for better outcomes.
– Disclaimer –
This blog is for informational & educational purposes only, and does not intend to substitute any professional medical advice or consultation. For any health related concerns, please consult with your physician, or call 911.
Read More Related Articles: